Breast cancer is the most commonly diagnosed cancer among women. Its incidence has alarmingly risen over the past few years in India with a change in lifestyle and urbanization.
Indian Council for Medical Research has quoted 1.5 lakh new cases of breast cancer in India, of which 70,000 succumb to the illness every year.
Women generally shy away from getting ‘screened’ — which is, in fact, an alien word to many. They are reticent when it comes to self-examination of their breasts, and many of them are unaware of how a lump feels.
In urban areas, 1 in 22 women is likely to develop breast cancer during her lifetime as compared to rural areas, where the ratio is 1 in 60.
It is highly essential to create cancer literacy among women in urban and rural areas, and equally crucial to review the awareness among Indian women of the various risk factors. The prognosis of breast cancer is quite encouraging if detected at an early stage. The awareness helps increase attention, early detection and treatment as well as palliative care for the disease.
Why We Need to Talk About It
The taboo attached to speaking up about breast cancer is perhaps the biggest obstacle that exists in its early screening and diagnosis today. We need to be more open about the issue — as is required for all women’s health-related issues.
Prominently talking about it on forums, creating and implementing government schemes and publicizing on radio and print media, are some ways that will help drive home the message to women and masses as a whole; that it is okay to talk about breast cancer, and wonderful to be detected early.
While a lot of private institutes and individual practitioners are promoting and spreading the word, they will always be judged for possibly having a motive of profit behind their actions. The government needs to endorse the need and benefits of the same.
Mandatory Screening = Early Diagnosis
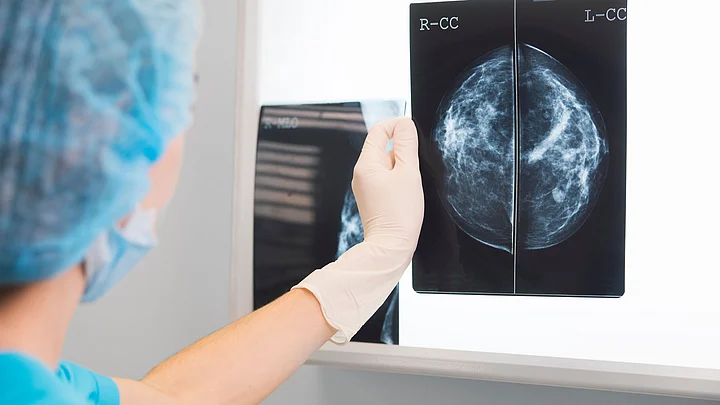
Many countries such as the USA, UK, Europe, Austria, and Canada have mandatory breast cancer screening. They have witnessed a dramatic improvement in the survival of breast cancer patients over the years.
While better medical care and advances have also contributed, it is undeniable that a large proportion is also due to increased awareness in the population, that translates into early diagnosis. In breast cancers, early diagnosis is a game-changer.
We have seen examples of the benefit in other countries and can contrast it with the rising incidence of breast cancer in India (even though in certain sections of the country, more urbanization could have contributed).
With the known benefit of early diagnosis, it is essential for the government to take initiatives for spreading awareness and bringing into practice the screening guidelines. We can then hope to see progress, as we did in the campaign against Polio and TB.
The government should partner with established private specialized cancer hospitals to accelerate adequate diagnosis with accurate treatment with their state-of-the-art technology. Providing treating doctors with uniform guidelines for the management of breast cancer appears to be an appropriate step forward in achieving this goal.
The main approach to prevention is to enable individuals to know what is required to reduce their own risk. However, currently, these messages are not targeted at specific at-risk groups or modulated in any way. Furthermore, policies aimed at general risk factors often do not identify breast cancer as a pressing disease which requires risk-reduction. Established screening programs enable early detection and treatment on a population-wide scale.
The current breast cancer screening guidelines are different in different parts of the world, depending on the disease patterns in those societies (multiple guidelines – ACR, USTFPF, ACS, ACOG, ACP, AFPP, NCCN).
As of now, we use the National Comprehensive Cancer Network (NCCN) international guidelines for screening. But it is highly desirable to have guidelines specified for our country, that would account for the different regions with different incidences.
The focus should be on prevention of disease development through health promotion, early detection (screening) and lifestyle management.
Implementation of a high-quality population-based breast cancer screening program is the need of the hour. And we, the doctors’ fraternity, are ready to shoulder the responsibility.
(Dr Upasna Saxena is Consultant of Radiation Oncology at HCG Cancer Centre)
(At The Quint, we are answerable only to our audience. Play an active role in shaping our journalism by becoming a member. Because the truth is worth it.)
